Let’s talk about sleep.
In our case, it would be no sleep.
Thing 1 goes through phases of (thankfully short-lived) poor sleep. Usually he quietly sneaks downstairs, steals the iPad, and falls back to sleep watching Thomas videos on YouTube. On the other hand, Thing 2 (our middle child and second son diagnosed with ASD) has survived on very little sleep for years. He is only 5.
(Image source: http://dailycaller.com/)
According to WebMD, “Researchers estimate that between 40% and 80% of children with autism have difficulty sleeping. The biggest sleep problems among these children include: difficulty falling asleep; inconsistent sleep routines; restlessness or poor sleep quality; waking early and waking frequently.” Thing 2 has all those symptoms. The alleged culprits behind poor sleep for autistic children include low tryptophan and melatonin levels, gut problems, sensory disorders, anxiety, mast cell activation, and Lord knows what else.
We describe Thing 2 as an anxious child. Changes to his routine and transitions are tough. He has always exhibited separation anxiety. He grinds his teeth constantly and makes aggressive (loud and long) vocalizations. He is like the Energizer Bunny and keeps going and going and going… We’ve battled poor sleep for a while, and adding melatonin at bedtime was our first intervention. While it made falling asleep peaceful, it never kept him asleep. At some point between 2:00 and 4:00 a.m., Thing 2 could be heard crying in his room or the hallway. We tucked him back in bed and told him to go to sleep. Sometimes that was enough; more often it was not. To protect the sleep of our other children on noisier nights, my husband or myself head back to bed with Thing 2 or let him sleep with us. At least we are kind of sleeping then, with a spastically flopping and whimpering kid by our side.
Thing 2 slept through the night a couple times this winter. Then we had constant night waking through spring and summer until August 1–the last time he slept through the night. He typically sleeps from 10:00 until midnight, then he is awake on/off and may sleep in bursts of 30 minutes to a couple hours. When our alarms buzz and it’s time to get ready for the day, Thing 2 has an epic meltdown because he is too tired to move. Mornings are miserable. Whether it’s lack of sleep or anxiety or something else, I don’t know, but he also no longer enjoys activities that made him happy. Now swimming and playgrounds and so many things lead to meltdowns.
You name it, we tried it. We maintain a bedtime routine, limit screen-time and noise, increased melatonin and switched to an extended release, supplemented l-theanine (for relaxation) and 5-HTP (to boost serotonin levels). Nothing made a difference. At his 5-year check-up this summer, I explained how sleep went from bad to worse and asked that Thing 2 be evaluated for ADHD or a sleep disorder or an anxiety disorder or all of the above. None of those would/could be done by our regular pediatrician, so she recommended we see the psychologist who performed the autism assessment. In the meantime, we gave clonidine a try. I hoped clonidine would be the answer to our prayers for more peaceful nights because many friends recommended it, saying it improved ADHD symptoms and sleep for their autistic children. The choice to medicate is difficult, even when it comes to supplements. I worry about the long-term or side effects of medications, but at some point it has to be an option on the table.
I called our psychologist’s office and was told she only does autism assessments, not ADHD or anxiety. I reached out to Thing 2’s teacher and BCBA for suggestions and got articles about sleep studies. I called a local special needs pediatrician and was told she was booked through March and there is a WAIT LIST for April appointments.
It’s September. And clonidine only made things worse.
At the end of my rope, I called our pediatrician and left a message that clonidine was ineffective, did we have other options, and could she pull any strings with that ridiculous wait list for the developmental pediatrician. The voicemail I got back: “This is as far as we go as pediatricians.”
That was the precise moment I snapped, and it was ugly. The floodgates that are my tear ducts opened, I called the office back and demanded to speak to our doctor because her message was unacceptable. I explained to her that we are in crisis mode, that Thing 2’s erratic behavior affects all parts of his day, and I am becoming the parent I never wanted to be: cranky, mean, yelling, impatient, and exhausted.
She’s getting us an appointment with a neurologist as soon as possible. For Thing 2, not me. But maybe I should also have my head examined.
It’s one thing to deal with autism every day and the ways that neurological disorder manifests itself. I realize it’s a journey with peaks and valleys, and that is fine. What deflates me is the lack of understanding we get from medical professionals. Autism is complex, and our kids are sick–some chronically. Whether they battle gastrointestinal problems, inflammation, seizures, feeding disorders, anxiety…couple that with learning disabilities, speech delays, processing and auditory disorders, and sensory sensitivity. My kids do not have the communication abilities to tell me what hurts, so we need real partnerships with doctors who can flush out these symptoms and bring peace to their little bodies. It’s time for the medical field and insurance companies to stop dismissing and disrespecting our problems as “that’s autism,” as if it’s an educational problem to tackle, and spend the time necessary to HELP our kids live healthy, happy lives. And these wait lists everywhere? Give me a break!
This kid is tired. So are his parents.
In other news, I’m breaking up with our pediatrician. And Thing 2 slept last night after a dose of hydroxyzine before bed. Hallelujah!! But me? I woke up every hour thinking, “Why isn’t he awake? What’s wrong? Is he still breathing? What’s happening?” It’s bedtime PTSD.


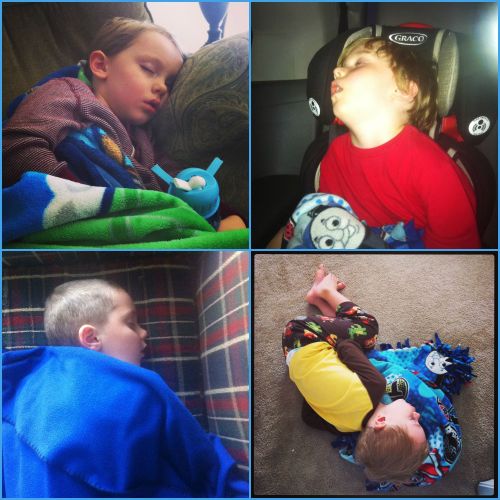
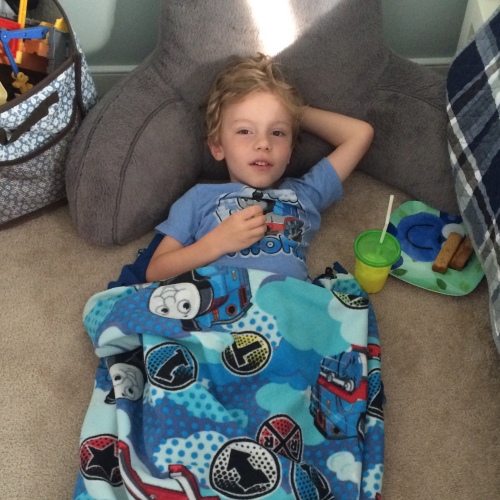
I would never guess when I see you every day at school that you rarely get a good night’s sleep. I can’t even imagine as I complained about two nights last week of not sleeping well. Keep fighting for you and your kids!
LikeLike
Ha! That’s because I’m at the coffeemaker 4, 5, 6 times a day. Thing 1 went through a rough patch last year, now it’s Thing 2’s turn. This, too, will pass. Until then, I drink a lot of coffee.
LikeLike
Im in awe of you.
LikeLike
Some of my worst parenting moments happen at 2:30 a.m. But thanks:)
LikeLike
Pingback: What’s Wrong with THAT Kid? | HONORED GENERATIONS
Pingback: Neurology… | Far Beyond Zebra
Pingback: Neurology, Part II | Far Beyond Zebra